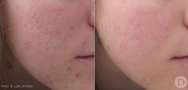
Treating acne requires comprehensive medical treatment and it is essential to consult your doctor or dermatologist.
Acne is a common chronic disease of the hair follicle associated with the sebaceous gland, characterised by enlargement of the sebaceous glands, along with the blockage of follicular ducts towards the surface of the skin and the consequent inflammation. There are several types of acne which appear mostly on the face, but can also on the chest, neck, back and upper arms.
Up to the present time, we have not yet fully discovered all the causes of acne. Recently, they have become more frequent in one’s mature years, in the third, fourth or even fifth decade of life. On average, acne lasts from 4 to15 years and has a considerable impact on the quality of life, on social life and self-perception, especially in the period of adolescence.
As effective treatment within the first two years following the onset of acne definitely reduces formation of the subsequent scars, one should consult a dermatologist as soon as possible. It is particularly important to decrease severe inflammation, to perform proper daily care based on medication (antibiotics, isotrethionine or contraceptives, if necessary) and special skin-care creams, to use light therapy (IPL or PDL laser) as well as to avoid sun exposure and sunbeds.
Treatment of acne
Treatment of acne requires comprehensive medical treatment, so it is essential to consult your doctor or dermatologist. Acne is a chronic skin condition that is treated by dermatologists. Innocent forms of acne, blackheads and whiteheads, can also be removed by an aesthetician, but more important is the treatment that prevents them from forming, calms the inflammation of the skin and prevents the scarring that occurs after acne inflammation.
Different forms of acne are treated using different approaches.
Mild acne:
- creams with benzoyl peroxide, tretinoin, clindamycin or adapalene,
- low-dose contraceptives (with drosperinone, cyproterone acetate),
- antiseptic wash gels, salicylic acid,
- light therapies (LED, IPL, PDL laser).
In addition to the listed therapies for mild acne, the following is advised in certain cases:
-
- taking a tetracycline antibiotic or azithromycin,
- long-term use of contraceptives with antiandrogens in women and in polycystic ovary syndrome,
- treatment with isotretinoin in the duration of several months in case of treatment failure,
- NEW: fractional radiofrequency treatment (Fractora).
Severe acne:
- in case of high fever, joint and bone pain, extensive inflamed skin lesions, hospital treatment is necessary,
- high dose antibiotics, anti-inflammatory drugs,
- isotretinoin treatment in the duration of several months.
Home acne treatment
When the number of inflamed skin lesions remains under 15, one can apply cleansers and creams to treat acne, which are available over-the-counter in pharmacies. If after 1.5 months of treatment the condition has not improved or the number of inflamed lesions keeps increasing, we suggest continuing the treatment with a dermatologist.
Acne scars
If acne has already left scars on your skin, fractional radiofrequency (Fractora) or fractional ablative CO2 laser can be used to improve the appearance of the scars, make them narrower, shallower and smooth the transition between the scar and the surrounding skin.
Acne occurs in both sexes of all races. They prevail in adolescents, with 16-18 year olds being the most frequent target group. Nevertheless, first-time appearance of acne can also affect younger children and people over 20 years of age.
Acne is caused by several factors:
- genetic influence,
- the influence of androgenes,
- skin bacteria,
- innate immune system and mediators of inflammation,
- sebaceous duct obstruction,
Exacerbation of acne can be a result of:
- polycystic ovary syndrome,
- drugs such as steroid hormones, epilepsy drugs, EGF inhibitors and other,
- applying greasy cosmetic creams and oils,
- high air humidity,
- high dairy products diets and high GI foods (simple sugars).
Most acne appears on the face, but it can also appear on the neck, back, chest and elsewhere on the body. The pilosebaceous follicle is the site in the skin where acne forms. They can appear in an inflammatory form as tiny red cells with or without a yellow tip, or as deep reddened indurations. Blackheads and whiteheads represent a non-inflammatory form of acne. It is possible to find several forms of acne in one person at the same time. Individual acne lesions may last less than two weeks, while deeper lesions may last several months. Most patients with acne have oily skin.
The typical clinical signs of acne are:
- open and closed blackheads (white and black comedones),
- inflamed cells,
- nodules and cysts – in severe forms,
- red-brown spots and scars,
- impaired social life and impact on psychological well-being.
Acne is divided into mild, moderate and severe forms according to the number of characteristic acne features:
Mild acne: the total number of all typical clinical signs is <30.
Moderate acne: 30-125.
Severe acne: >125.
Usually, but not always, acne is most pronounced in the teenage years. There are several theories for this:
Higher levels of sex hormones during puberty
- Sex hormones are converted into dihydrotestosterone, which stimulates the sebaceous glands to increase their volume.
- The sebaceous glands produce more sebum and the sebaceous gland cells produce more pro-inflammatory substances.
- Inflammation and improper shedding of hair follicles clogs the sebaceous ducts, which makes a blockage, resulting in the formation of the blackheads or comedones.
- The wall of the pilosebaceous follicle is perforated, which increases inflammation in the surrounding area.
- The inflammation is also influenced by bacteria in the follicle → an inflammatory lesion is formed in acne.
Although acne is most common in teenagers, it can occur at any age. It usually subsides by the age of 25, but 15 % of women and 5 % of men have acne after the age of 25. It is not uncommon for them to appear for the first time in adulthood.
Photo gallery
Appointments and further information
To book an appointment, contact us Monday to Friday from 8:00 to 16:00 on the following telephone number: 064 12 80 15 or send an e-mail: info@derma-rogaska.si